We are trying to conceive (TTC), yet again. This time trying for baby #3, Lord willing. I can’t help but reflect on how different my experience is now than it was in 2015. God has already blessed us tremendously with 2 children that I wasn’t sure we would ever have. One child was blessed to us with the help of IUI. Our second child came completely naturally shortly after beginning to try. We are asking yet again for a child, but this time with a much greater peace of mind that we will diligently do our part and wait for God’s answer. A goal we were striving to achieve the first go-around and seemed so far out of reach. This isn’t a blog about TTC, however, it’s a blog post about my health and the journey back to seeking my own best health (and thereby, my best fertility). I want to tell you my story of how 4 years of infertility services and the detour that we made to focus on having children did nothing to address my health concerns. In fact, they didn’t even help me be at my best fertility.
In this new phase of my life, I have renewed my focus on my own health and resolving my serious women’s health concerns that were cast aside for almost 5 years. I’m so grateful for this window of time to resolve some long-unanswered questions. I’m hopeful that if you can relate in any way to my experiences, that you find some inspiration and resources to learn more about this incredible body God gave to women and how you were designed to feel your best, whether seeking to make babies…or not! You deserve your best health!
So let’s back up…our story of infertility had a weird start. We were not trying for children at the time. I was incredibly stressed and attempting to manage our incredibly hectic life as newlyweds (married about a year), a challenging military job where I often worked too many hours, and the other extras that I always seemed to add to the list. My health was suffering. I got stress-induced shingles at 26. Then I was having tons of seemingly random symptoms and they all seemed eerily linked to my cycle as I began to notice the trend. I went to the doctor searching for answers.
I must have seen 10 or more different specialists. I know some of you have been there…maybe it’s the GI tract (colonoscopies and all), maybe it’s autoimmune, maybe it’s neurological, maybe it’s psychological, maybe it’s lifestyle: diet, stress, etc. I did receive some welcome help when they began looking into my sleep, which is a separate topic, but unfortunately, not the answer to the issues I was investigating. I was placed on thyroid medication to “see if it helped based on my symptoms” despite being within the “normal” range with my blood work. It certainly helped a little, but still no real answers. Back to the OB with almost nothing to show for it except for a list of what was not wrong. So, when all else failed, maybe it’s endometriosis. Take Motrin all the time in case an episode of painful cramping occurs, I was told. Or go see a specialist for a more thorough investigation.
I wasn’t satisfied with the open ended, not helpful “treatment plan,” so I decided to see a specialist. Which resulted in my next problem. Very few doctors specialize in endometriosis, except fertility centers with a focus on infertility treatment. It breaks my heart in retrospect that a condition that results in severe pain for women for most of their reproductive years is typically addressed only when pursuing children. Why is a condition that is so linked to our reproductive window only relevant when we want to actually tap into the ability to reproduce? Our body is dealing with the often painful symptoms the whole time. But I digress…
So a fertility center was our next stop. I dealt with some difficulties in healthcare coverage in my attempts to explain that this was not infertility treatment, just women’s health care and should be covered. Whether in the military healthcare system (which I was) or the private sector, I know many agree that this is a tremendous headache all on its own. We found a place that was covered by Tricare (military healthcare). I hate the way all it played out from there, but it’s a part of our story for a reason.
At the clinic, they recommended exploratory surgery for endometriosis and to check on my Fallopian tubes at the same time. At this point, though it wasn’t my reason for being there, I was starting to get very nervous about our potential family planning. I definitely wanted a family and was itching to start much more than my husband :). I was on my latest form of birth control (BC) at the time, an IUD. I had been on different forms of BC since 8th grade due to horrible symptoms during my cycle. Cameron and I agreed to start trying to conceive right away if we found out about any barriers to fertility during our investigations into my health. So the IUD would come out also while they were there.
Oh by the way, office policy is that you must take a male sample as well…since it’s a fertility clinic, so we did that (out of pocket) because they told us too. I certainly wasn’t upset about looking into this troublesome possibility.
I had the surgery, then went to the follow-up appointment with my mom. The doctor began to explain his findings. He did not find endometriosis. I’m not convinced he checked the areas I requested based on my symptoms, but as far as we could tell, that was a dead end. It might be endometriosis and we didn’t find it. It may be some scar tissue from an appendectomy when I was young. But all was in good working order as far as they could tell. He made sure to caveat the good fertility news with his prediction that though both my tubes were “open” that the tube with scar tissue surrounding it wouldn’t be ideal and may hinder our chances for children overall. At least one working tube, great news, right? Sure, except that I still had no answers to serious health issues that seemed perfectly tied to my cycle at this point.
It was such an awkward day…as I sat there with my mother trying to process all of my health concerns, the doctor chose to deliver the news about the male sample taken earlier. He was apparently not dissuaded from this despite the fact that Cameron was not there.
Unfortunately, the numbers did not look great from the sample. He proceeded to tell us his medical opinion that the sample looked very troubling and that we needed to retest. I called Cameron after the visit, who of course was concerned with the news about my health, and had to bombard him with news we were never seeking out. I didn’t know how to handle the whole circumstance and it was so uncomfortable having to relay news like this to him. I was unsure of how he would react. He took the news well as always, with a bit of skepticism about the doctor’s opinions and obliged another test.
All conversation about my health frankly stopped that day, in part because of me. The doctor had nothing more to say to me about my painful symptoms. We didn’t find anything, who knows what’s wrong, but your reproductive organs should work…now onto your fertility as a couple. I’m sure not every fertility clinic is like this, but since this was our first experience of this kind, we didn’t have anything to compare against. And he gave us some really bad news about our fertility as a couple, which completely overtook me. I was content to set aside my own health since the doctors couldn’t help, especially in light of the tragic new problem that we had uncovered. So many of my hopes and dreams in this life revolved around having children and I was ready to follow that detour.
At the second visit with the doctor, I was prepared and Cameron was with me. He told us that the second sample was worse than the first and that “miracles can happen,” but he predicted we would not have children without help. Luckily for us, of course, they offer IVF (In Vitro Fertilization) so we could pursue that. Take as long as you want. We are available when you are ready and here is our pricing sheet.
I’m so thankful for the strength of character of my husband. Cameron is not willing to let anyone define things for him. He was also not willing to jump to the best chance solution for children without looking into everything first. He doesn’t let his emotions lead, no matter how few they may be :). He is always calm, rational, and un-rushed. That was the only reason I wasn’t carried immediately into a chase to yield a child from day one…because my heart was broken and I wanted to regain a better chance for children right away. Although my health issues didn’t seem to be contributing to my fertility (and yet I found out later, they did), we were still dealing with infertility as a couple and I still felt like crap.
It’s not to say that the news about infertility problems on Cameron’s side was completely smooth. We had to work through the news and stretch ourselves and our marriage a lot. His concern was not that he was any less of a man if there were fertility obstacles, but more about whether I would be happy with “just him” if he couldn’t give me children. Marriage is filled with difficult questions like that. I would have loved to be able to convincingly say, “YES! Of course our marriage is enough!” and yet my heart was breaking over the sadness that many of my hopes and dreams regarding children were beginning to feel impossible. I had never considered the possibility that children would not be in my future, whether by adoption or naturally. I had never considered a marriage without children. And I didn’t want to. Despite my difficulty in answering these questions well, my husband reminded me that children are not a requirement for heaven. I held on to those words for a long time to ground me as we struggled forward.
Nonetheless, I desperately wanted to convince Cameron to shorten the timeline of trying on our own and pursue IVF right away. How about only 6 months, 3 months…please?!! Cameron slowed me down. Whatever we are pursuing, it’s with a different doctor. What is the IVF process like? What does it entail? Does the Bible speak to this sort of thing or anything like it? How comfortable are we with creating life through an artificial process?
I can’t say I handled all these questions with grace. It was more likely with much resentment. And yet, he wasn’t wrong. We needed to look into it. We needed to give it time. So we started trying to conceive on our own. Despite still feeling painful symptoms throughout my whole cycle, adjusting to my unsuppressed cycle again after removing my birth control, and the news hanging over our heads that conceiving children naturally was probably not going to work, we tried for a year.
I learned about charting my cycle with several Fertility Awareness Based Methods (FABM) during this time. I learned way more than I ever thought I would know about ovulation and the reproductive cycle for women. I learned that my body would naturally tell me when I was ovulating and I didn’t need to spend money on ovulation predictor kits. I also noticed my symptoms rise and fall with the key times of my cycle. Not only that, but I experienced persistent cramps, which turned out to be painful ovarian cysts that didn’t go away naturally for months. Almost amusingly, it was my spine specialist who actually found one of the cysts, not my OB. So many more problems, but they felt normal to me. And I was told they were normal.
In the meantime, we wrestled with our comfort level with IVF. I’ll save most of that for a separate post, because it is in many ways, its own story. Ultimately, Cameron decided that he wasn’t comfortable moving forward with IVF and though I agreed with his rationale, I was struggling to let go of what seemed like our only hope for children.
I went to the doctor for a typical women’s checkup. I had long ago accepted that my health had no answers and I expressed that we had been TTC for about a year. For any of you that have been there, you know that 1 year is the magical number that labels you as having “infertility.” The doctor kindly gave me information about a military hospital in San Diego that has an infertility clinic that I could get referred to where they cover most of the cost. I can only imagine the additional stress of having to pay for these services, which most insurance plans don’t cover. For many, the dream already seems so far off and then it comes down to how long you can financially keep going as well.
So we optimistically received the referral, which put us on the waitlist for IUI (Intra-Uterine Insemination)! Cameron likes to summarize IUI by saying, “his guys get on a bus and go straight to the party.” We had agreed to approach infertility treatments with one goal in mind, only seeking to address known medical issues and no more, even if it would give us better chances for a child. I’ll go into this more in the fertility treatments post.
I had a bit of renewed hope that someone would try to connect the dots of my difficulties tied to women’s health since I was going to an infertility clinic. Unfortunately, most fertility clinics are essentially just Artificial Reproductive Technology (ART) centers, which means, they are in the business of making babies. This was not an avenue to find answers to health concerns. Nothing about that goal is inherently wrong, but it is an important distinction. This was an ART center. Not a moment was spent on my health. Every moment of our time there was spent setting up, preparing for, and proceeding with the IUI process.
We presented the doctors with Cameron’s sperm analysis results, indicating that we already knew much of the reason for our infertility and the doctor shocked us both by saying that he didn’t think they were “that bad.” He had seen far worse numbers with successful, natural pregnancies. My heart sank for the reality of what this good news meant. I convinced myself for the entirety of our TTC on our own that it was likely impossible and this second opinion indicated that it was never as dire as we were led to believe. So…get a second opinion! Don’t let your hope be diminished from one opinion.
We began the IUI process very hopeful and yet my health got worse. WAY, WAY worse. According to the process of the clinic, they would place patients on birth control to pause their cycle until they had appointments available so that their calendar wasn’t dictated by each woman’s natural monthly rhythm. An understandable problem. Except I have never done well on birth control and have had to switch to multiple alternatives to find one that had the least negative impacts. I wasn’t even on fertility hormones, just birth control at first and I was in the ER twice with heart palpitations. I was asked if I’d ever had panic attacks before (no but I also don’t deny it could be that). I was referred to a cardiologist to check out my heart (my heart was fine). And yet, through it all, I was given full assurance it couldn’t possibly be the birth control. Still, since I couldn’t find any other reason for the new symptoms, I refused to take birth control anymore. I told them if my window would not fit in their schedule, I would miss that cycle rather than start and stop my body’s natural rhythm for convenience. Magically, the heart palpitations stopped.
After our 1st failed IUI attempt without hormones, the doctors mentioned that the thickness of my uterine lining wasn’t ideal, though low-normal. I didn’t even think to ask why my lining might be thin (also connected). It was simply an obstacle to the best possible results to IUI. So we added hormone treatments for me to address that medical concern and all the crazy hormone symptoms that come along with it. 2nd failed IUI. 3rd failed IUI. And more health problems.
Finally, I had to stop. As much as it pained me to take a break and lose 3 chances to conceive a child for free, I couldn’t take it anymore. We decided to take a break for 3 months and go back to TTC on our own. After the pause, I came back refreshed-ish and extremely done with delaying our best chance that we were comfortable with as a couple, so we tried IUI again.
The 4th IUI experience was more relaxed and even fun. We combined the procedure with a fun getaway weekend in San Diego. We were laughing with the staff and simply more at ease. Whether we were successful or not, it was a great memory.
Fast forward through the dreaded 2 week wait. Because hormone treatments take over your natural cycle, you are discouraged from trying to understand your body and the symptoms you experience. You can’t feel if you are pregnant, you just take a test. I was ignoring my body’s symptoms since the medications were in control. I took a pregnancy test assuming it would be negative, simply so I could move on to start the next round of IUI steps and the test showed positive!!! I was in tears thanking God for this gift! We heard Carson’s heartbeat at 5.5 weeks of pregnancy…that is about 24 days after conception…absolutely incredible. The doctor felt confident that the pregnancy was strong and I was told to report to my OB at the appropriate time (10-12 weeks pregnant). I was so fearful about losing my baby despite all the good news we had. I had no information about statistics for ART babies. I had no idea if my women’s health concerns would lead to problems during pregnancy. I simply had a baby and was placed back on the typical pregnancy track. All infertility indicators no longer mattered because we successfully achieved a pregnancy.
In many ways, I had an easy pregnancy physically. In many other ways, I had a difficult pregnancy mentally. Ultimately, I was so overjoyed with the outcome, that I don’t think the negatives upset me almost at all. But they were there. Carson surprised us 3.5 weeks early and this Mama was caught extremely off guard. I like structure and planning and my introduction to motherhood was a reminder that I am not in control of this. That has been a recurring lesson for me on this journey. I later found out that ART babies very often come early.
I’m going to fast forward quite a bit here to trying for child number two. Once Carson was about 8 months old, I asked that we begin trying again. Not because I wanted children 15 months apart, but more because I worried it would take a long time again. However, I had more confidence that we could succeed after the 2nd opinion on Cameron’s sample. I heard that your chances for a second child can be better so I was optimistic and worked to convince myself that “I can get pregnant.” Because I was out of the military now, my stress had significantly reduced. I was feeling a lot better health-wise. I was working out and in a better balance with food and tracking my cycle. In not even 4 months, I was pregnant. Once again, shock! All those terrible odds…and pregnant, just like that! It didn’t even occur to me to be daunted by the idea of 2 children less than 2 years apart.
So here comes baby #2 and I am titled “high-risk” because of my early delivery with Carson. Without any discussion from my doctor, I received a call from the pharmacy about a progesterone shot that I would need for weeks 16-36 of my pregnancy. This news was incredibly hard for me to process and I never received any real explanation why I would need progesterone except that it would help avoid early delivery. This process was borderline traumatic for me as someone who likes to be prepared and thoughtful about all decisions about my body and my baby, but I dealt with it and set up the appointments.
My pregnancy with Quinton was extremely stressful. I was constantly worried about him coming too early and had prodromal labor at 35 weeks. Cameron wasn’t allowed to leave town for the last 2 months. My family drove up and back due to our first early labor scare. And after all that, he was born 1.5 weeks late after inducing me to labor by breaking my water. There’s that reminder that I don’t control things again.
When Quinton turned 1.5 years old, we slowed down on nursing. I decided to stop my thyroid medication to see how my body handled it. After all, I was placed on it for many symptoms that had subsided. At first, I felt ok with all the adjustments as my body sought to rebalance. However, my cycles were looking very odd and my symptoms were getting worse again. I blamed it on nursing fluctuations of my hormones until 3 months had gone by and I saw no improvement. So I went to the OB again.
Bloodwork normal, ultrasound normal. Maybe you have an infection, so take preventative antibiotics (which caused a different problem) and that was it. No answers. No need for followup. I was right back where I started 5 years ago.
Finally, I had had enough. Quinton finished nursing and the problems persisted. I wanted to finally figure this all out. Why did I feel so terrible all the time? Why was it all so rhythmic? We were trying on and off, but I was no longer as worried about whether we would have another baby, I just wanted to feel better and find some answers.
I found an online convention about “Unexplained Infertility” and decided to check it out (https://www.unexplainedinfertilitysummit.com). I was overwhelmed with what I found. Many stories of ART disappointments and no answers to health concerns and an overwhelming emphasis on listening to your body and working towards your best health…in which your best tool to investigate with is your natural cycle. Not only did these approaches help women find answers to their health problems and understand their bodies natural rhythm, but they often had success in pregnancy despite multiple failed IVF cycles.
So I began to dig in. I hired a charting coach to really hone in on my ability to understand my cycle. It’s almost amusing to me to consider how well the bodies God has given us are designed to work. I found a Restorative Reproductive Medicine (RRM) doctor’s office, which I had previously never heard of. I told them that all I really wanted was to get to the bottom of my health issues. I know I can get pregnant now. Yet something is very off.
They helped me to determine that I actually do have a thyroid concern by taking my hormone levels at the right time in my cycle and studying the detailed results. Check out how much your hormones change throughout your cycle…
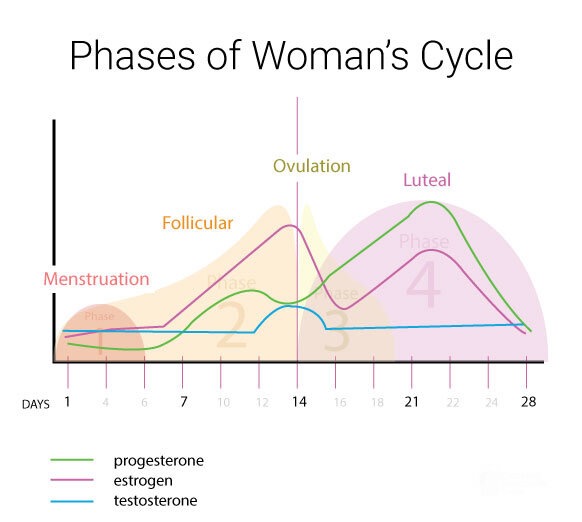
They also helped me confirm something that my charting was already showing…I had low progesterone—almost half of the desired amount at its peak. Despite being in the normal range for typical bloodwork and being thoroughly tested at a fertility center 5 years earlier, I had never known this. And it explained 95% of my symptoms over the years spanning all the way back to my very first cycle, before I was placed on birth control to suppress the reproductive process. All those years of cysts (likely due to insufficient progesterone) and not one indication of the underlying problem. All those symptoms. I was even put on progesterone simply as a known preventer of early delivery without linking this up.
Low progesterone is the leading cause of miscarriage, though I gratefully haven’t experienced one (and yet I know so many who have and I grieve with them). Low progesterone can be determined with as little as 3 months of charting and a blood test at the right time in your cycle to confirm. You can investigate these things at whatever point your body starts indicating that something is off! YOU DO NOT NEED TO BE TRYING FOR CHILDREN TO KNOW IF YOU HAVE LOW PROGESTERONE! Yet, this is often the timeframe when women find out they have this concern. In order to be diagnosed with “infertility” related to miscarriage, you need to have experienced at least 3 miscarriages. The first 2 are not considered sufficient indicators. And their recommendation is usually to override your cycle just long enough to get you a baby.
I wish that I had looked into these problems when I first began to have difficulties with my cycle. I didn’t know anything about the way my body worked then and frankly, most of the medical community didn’t either. RRM is relatively new and considered a more holistic approach to your health. But now I want you to know, if you’ve made it this far, there are answers! Your cycle is actually your greatest tool in helping you achieve your best health! What a gift it would be to young women to help them investigate why their health is not ideal and help them to feel better for all the years before they want to start trying for children. Most women’s health concerns are not solely problematic for fertility. They are often problematic for their entire reproductive window.
I fear that so many women are like me. That they never found answers to their health difficulties and then later were faced with infertility stuggles. They are dealing with hormonal swings of ART medications all while being told that their best chance of having a child is only by overriding their body’s natural process. Their health is irrelevant to the process of getting pregnant. Their fertility health is only relevant to the extent that it prevents them from having a baby, not for the other exponential health outcomes.
I am grateful for this time to examine my own health without the hormonal swings of another pregnancy and the gap in investigating my cycle. While I would happily be interrupted from my investigation to have another baby, this time has been its own gift. As much as I desire more children and am so grateful for the children I have, I am sad that I shelved my own health to chase my dream for children for so long. I’m even more sad knowing how little of my own health and natural fertility were at the forefront of the entire infertility process. I finally feel like my priorities are in the right order. I finally found answers to questions almost forgotten for being ignored (even by me!) for so long. I finally feel like I am working towards better health…and as a result, my best fertility. I am preemptively improving my progesterone levels for my health and for my fertility and decreasing my chance of miscarriage. I finally realize how beautifully the body God gave women is designed to work. I finally am beginning to understand the natural metric of my cycle instead of pausing it, ignoring it or suppressing it. Finally…

[…] find any endometriosis (later contradicted by a women’s health surgeon who did remove it—see this post or this one), but assured me that my tubes worked despite extensive scar tissue from a childhood […]
LikeLike